 At this stage there is very little cartilage left and there are very large bald patches (i.e. the tyre is bald).
At this stage there is very little cartilage left and there are very large bald patches (i.e. the tyre is bald).
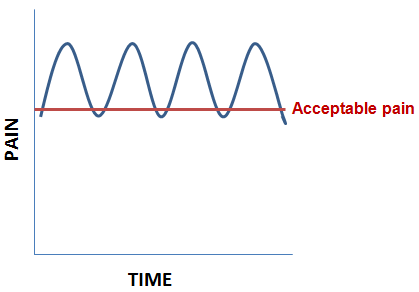
Symptoms: Constant ache/pain often severe affecting the whole knee or hip. The area may be swollen, thickened, stiff and there is often pain on weight bearing. The muscles may look smaller and feel weak.
Key points:
- Take medication regularly as prescribed
- Use a walking aid
- Keep to an ideal weight
- Try to keep active and do the recommended exercises
Treatment options
Your GP may repeat the X-ray of your joint and reassess your symptoms to establish if you have reached the stage where a surgical opinion could be beneficial. If not already, they may offer a steroid injection into your joint. Before considering surgery they will need to assess how severe your symptoms are using a questionnaire, whether you are using all your pain relief medication regularly, have already accessed physiotherapy, that you have a healthy weight or are working towards it, and, if you are a smoker, that you are offered help and support to stop smoking to increase your chances of a healthy recovery following surgery.
Obesity is the single most preventable contributor to Osteoarthritis for weight bearing joints. For every pound of extra body weight you may be carrying the increased loading on the knees/hips going up stairs equals 4 pounds – so for every 10 pounds overweight you are your knees will have to take 40 pounds extra load.
If you are overweight it is best to address it with a combination of healthy eating and exercise. Help with this plan can be accessed from groups such as Weight Watchers, Slimming World or the local council “Fit 4 Life” program.
Fit for Life program
If you are over 18yrs and have a Body Mass Index (BMI) of 25 or above Harrogate Borough Council offers a free 12 week service called “Fit 4 Life” (funded by NYCC Public health team) which combines Nutrition and lifestyle advice with exercise sessions. These programs are offered at venues across the Harrogate district during the day and some evenings. You can find an up to date timetable here.
The “Fit 4 Life” programme is made up of group sessions consisting of individual weigh-ins, physical activity and weight management advice, covering different topics each week including:
| Goal setting | Behaviour change |
| The “eat well plate” | Salt |
| Portion sizes | Benefits of physical activity |
| Eating awareness | Eating out |
| Fats Food labelling | Drinks |
Before taking part in the group session you will be required to attend an induction with the instructor. This will include a basic health check, a health questionnaire and general chat about your lifestyle.
For more information about the Fit 4 Life programme call 01423 500600 (ext. 58382)
At Level 3 stage you may find that exercising is very uncomfortable, however it is still very important and physical activity is the best non-drug treatment for improving pain and function in OA. Try to do gentle exercises every day and this will help to reduce the swelling and pain. You will also be keeping your muscles strong to protect your knees/hips.
What Exercises Work Best for Osteoarthritis?
- Range of motion exercises can help maintain and improve the flexibility in the joints.
- Aerobic/endurance exercise strengthens the heart and make the lungs more efficient. This conditioning also reduces fatigue, controls weight and builds stamina.. Aerobic exercises include walking, cycling, swimming or using the elliptical machine.
- Strengthening exercises help maintain and improve muscle strength. Strong muscles can support and protect joints that are affected by arthritis. You can find a list of suitable home-based exercises recommended by Arthritis Research UK using the links below:
- Knee pain exercises
- Information and exercise resources
How do I become active?
You will benefit from most exercises although we would recommend that you do not do high impact activity i.e. running long distances on a road surface. Locally Harrogate Borough Council run exercise programs and you can find the information by emailing [email protected] or visiting the sports development section of Harrogate Borough Council Website.
If you are getting pain from your joint when walking/ weight bearing you could benefit from a walking stick. The walking stick will take some of your body weight through the hands reducing the load on the lower limb joints
There are several walking aids but in the early stages of OA a walking stick is the most appropriate. They are suitable for most people and easy to walk with.
Measuring a stick
When on the floor the handle of the stick should reach your wrist when your elbow is very slightly bent.
Using a stick
When walking with a stick use one stick in the opposite hand to the affected leg. Put the stick and the affected leg forward together.
Instruction
There are many web sites which give instructions on how to measure for a walking stick. Here’s one example:
Supply
Walking sticks can be purchased from Yorkshire Care (Forest Lane Head, Harrogate: 01423 799960) / walking shops/ garden centres/ some pharmacists/ Sports Direct etc. Your GP could also request one to be issued from the Physiotherapy department if you need help with balance or learning to use one.
If you have reached level 3 on the pathway, your osteoarthritis is now affecting you significantly. You may need to progress from a walking stick to a walking aid which provides more support.
Crutches: Crutches can be used if you need more support for walking and taking body weight. These are generally only required in the later stages of arthritis and not all people need this level of support. Crutches are issued by the Physiotherapy department at Ripon and Harrogate District hospitals.
Frames:- Walking frames are rarely required for osteoarthritic people unless they have more than one complaint. They give a lot of support and help with balance. You should be given advice on how to use a walking frame before using one.
These are available from
Yorkshire Care, Forest Lane Head, Harrogate (01423 799960) and the Physiotherapy department (with a doctors referral) as above.
It is normal to feel down about your arthritis. Negative feelings when dealing with pain and loss of function are normal but these can lead to depression and anxiety. Twice as many people with arthritis experience anxiety, compared to the general older adult population.
If you have negative feelings such as these do not struggle on your own. You can seek help and discuss the problems with your GP, Practice Nurse or even family and friends. All these conversations will help you deal with your emotions and they may lead to a more positive way of managing the problem.
For moderate to severe pain from osteoarthritis, try applying heat and cold to the affected joints. Experiment with these heat and cold techniques until you find what helps you most.
Heat
- Apply heat 2 or 3 times a day for up to 20 minutes, using a heating pad, hot shower, or hot pack. Heat seems to be effective for pain and stiffness related to inactivity of a joint
- If you are using an electric heating pad, avoid falling asleep while the pad is on. If you think you might fall asleep, set an alarm clock to go off in 20 minutes. Use heating pads set on low or medium, never on high
- If you are using a microwaved wheat bag make sure that you shake it before putting it on your skin to prevent any hot spots
- Try alternating between heat and cold
- After a heat or cold treatment, try some gentle massage/ rubbing for relaxation and pain relief
Ice
Ice and cold packs can relieve pain, swelling, and inflammation from injuries and other conditions, such as arthritis.
Types of ice and cold packs
| Ice towel | Wet a towel with cold water and squeeze it until it is just damp. Fold the towel, place it in a plastic bag, and freeze it for 15 minutes. Remove the towel from the bag and place it on the injured or sore area. |
| Ice pack | Put about 1 lb (0.5 kg) of ice in a plastic bag. Add enough water to barely cover the ice. Squeeze the air out of the bag and seal it. Wrap the bag in a wet towel and apply to the affected area. |
| Cold packs | Bags of frozen peas or corn are inexpensive, last 10 to 20 minutes, and mold well to your body. You can also buy cold packs that can be reused. Store them in your freezer. Some of are designed to wrap around an area, such as a knee. |
Using an ice or cold pack
Apply an ice or cold pack to the sore area up to twice a day for as long as you have pain, swelling, and inflammation. Use ice for 15 to 20 minutes, 2 times a day
Always keep a cloth between your skin and the ice pack, and press firmly against all the curves of the affected area. Do not apply ice for longer than 15 to 20 minutes at a time, and do not fall asleep with the ice on your skin. It is best to check your skin every 5 mins to make sure that you are not getting an ice burn.
Are you ready for surgery? Click here to find out more.
Hip: http://www.orthopaedicscore.com/scorepages/oxford_hip_score.html
Knee: http://www.orthopaedicscore.com/scorepages/oxford_knee_score.html